Exploring the array of value-based reimbursement types for FQHCs

Value-based care is marching across the healthcare industry, significantly altering the way providers get value-based reimbursement for the care they deliver.
But value-based care isn’t one single, unified program that looks the same across all payers and provider types. It’s a patchwork of alternative payment models (APMs) applied unevenly throughout the care continuum.
The value-based reimbursements available for community health centers (CHC) might be wildly different from those aimed at hospitals or specialty physician practices. Each model has its own clinical and financial goals, and individual payers may rely on their own proprietary mix of reimbursement structures to provide incentives for participants.
Navigating this infinitely varied landscape isn’t easy, especially when trying to decide which opportunities are most appropriate for a CHC or FQHC. To begin the process, it helps to know what types of reimbursement structures are available and what they will require from the organization.
(And if you’d like more help understanding the value-based care landscape for FQHCs, download our guide.)
Here are the five main types of reimbursements, ranging from traditional fee-for-service all the way to complete capitation.
5 main types of value-based reimbursement models for health centers

1. Fee-for-service
Fee-for-service (FFS) has been the dominant form of payment in healthcare since time immemorial. When a provider delivers a service, they get reimbursed for a set amount for that service. The more services delivered, the more payment received.
Fee-for-service is simple, but it has become unsustainable. FFS structures can incent providers to pile on unnecessary tests and procedures so they get paid for doing more, regardless of whether or not the services are beneficial for their patients.
Over-reliance on fee-for-service is one reason why healthcare in the United States is so shockingly expensive, yet outcomes continually rank among the worst in the developed world.
Value-based care is designed to change that, and it’s picking up steam across the industry. In 2020, only about 40 percent of healthcare payments still flowed exclusively through FFS arrangements with no link to quality or outcomes, according to the Health Care Learning and Action Network (HC-LAN). An additional 20 percent contained some performance-based requirements but were generally still rooted in the fee-for-service structure.
While most state Medicaid programs have embraced a form of capitation known as managed care, fee-for-service is still prevalent in many regions. Almost all states leverage FFS to some degree, making it important for CHCs and FQHCs to stay in touch with what this foundational payment technique means for their patient populations.
2. Upside risk
Upside risk, also known as one-sided risk, is the first step toward a value-based reimbursement partnership with a payer.
Upside risk models are built on fee-for-service architecture: participants still receive set payments for the services they deliver. However, in upside risk models, providers are also given specific clinical benchmarks to meet, such as ensuring that a certain percentage of attributed patients with diabetes have their A1C levels under control.
If the provider can achieve these goals while holding the costs of care below a complementary financial target, they get to keep a portion of the difference. This is known as shared savings.
If the provider doesn’t meet the agreed-upon cost threshold, they don’t earn any shared savings – but, crucially, they are not liable to pay back the excesses to their payer partner.
For this reason, upside risk is generally considered the “safest” entry point into value-based care. It provides opportunities to earn additional incentives but protects participants from significant losses if they still have more work to do on their practice transformation efforts and population health management techniques.
Historically, many of the value-based care programs from CMS and commercial payers have starting with upside risk and progressed to downside risk across a number of years.
3. Downside risk
Upside risk may be a good place to start, but downside risk is what payers are really after. Downside, or two-sided risk, does require participants to return a relatively limited percentage of the shared losses to the payer when providers miss their targets.
CMS is now using its policy levers to push the industry toward downside risk at a much faster pace. For example, the new ACO REACH model, as well as the large and influential Medicare Pathways to Success program, prioritize two-sided risk after years of evidence showing that accountable care organizations (ACOs) produced savings for Medicare while improving quality for patients.
However, not all providers are pleased with this direction. Downside risk is, after all, riskier for providers, and it can be challenging to successfully engage with these models without the right technologies, clinical strategies, and operational support.
Nonetheless, efforts by CMS and commercial payers to encourage downside risk are working. In 2020, 11 percent of all industry payments moved through downside risk models built on a fee-for-service foundation, says HC-LAN. An additional 7 percent flowed through even more advanced payment structures, including full and partial capitation models.
CHCs and FQHCs can do very well in downside risk arrangements, particularly in Medicaid, if they work with the right partners to help negotiate favorable contracts, prepare for clinical and financial changes, and build an ecosystem of success.
4. Bundled payments
Bundled payments, also known as condition-specific capitation, provide a single flat-rate payment for an entire episode of care. Popular in the specialty and surgical realms, bundled payments work best for treatment plans with a clear-cut beginning and end, such as a joint replacement or chemotherapy for a low-risk cancer.
Similar to other risk models, providers can keep the differences between the payment amount and the actual cost of care. But unlike with traditional downside risk, there is no cap on the amount of money the provider can lose if they exceed the payment amount. The practice is fully responsible for all of the losses they incur from overspending on an episode of care.
To avoid scrimping on care, providers are still given clinical quality targets to meet. This ensures that patients receive all of the services they need to achieve positive outcomes while still incenting providers to find new efficiencies and stay one step ahead of patient risks.
5. Full capitation
Bundled payments are just one step away from full capitation, which often takes the shape of managed care in the Medicaid environment.
In fully capitated models, providers receive a flat rate payment to manage a member’s entire constellation of healthcare needs for a given period of time. Providers must still meet quality benchmarks and can even receive additional bonuses or incentives for going above and beyond their quality goals.
This strategy provides very strong motivation for practices to inventive in preventive, proactive primary care. By keeping patients healthier for longer, practices will spend less on avoidable care and keep more of their reimbursements.
Many capitation models use a “risk pool,” or a percentage of the capitation amount that’s withheld from the provider, to mitigate the health plan’s losses or to pay for specialty services for the attributed population. If the health plan doesn’t end up dipping into this pool too heavily, the money is paid out to the participants. In the case of poor financial performance, however, the plan can take the money for themselves to pay off their expenses.
Medicaid is a largely capitated environment, and both CHCs and FQHCs are intimately familiar with the challenges of working in this world.
However, they don’t have to be limited by the constraints of capitated payments. Other value-based care models, including upside and downside risk structures, can actually enhance a health center’s ability to enhance their revenue through incentives and shared savings.
IPAs open a path to new financial models

Joining an independent provider association (IPA) is the first step toward being able to harness the potential of the rich and varied value-based landscape. IPAs can help CHCs and FQHCs identify the most promising opportunities and open up new contracting options that may lead to much-needed financial resources.
Especially in the wake of cuts due to HR.1 (also known as the BBB), CHCs need community connection and alternative pathways more than ever. As Cesar Herrera, CEO and Founder of Yuvo Health puts it, "With HR.1 going into effect, community health centers are set to face major funding cuts just as millions of Americans lose Medicaid coverage. Funding pressures are real, and they underscore the need for CHCs to consider new strategies.
"Value-based care offers a new path forward and one that finally recognizes the essential work CHCs have been doing for decades. These arrangements incentivize providers to keep patients healthy – connecting them to primary care and keeping them out of emergency rooms – which not only leads to better patient outcomes, but greater savings for the system and new revenue streams for the centers."
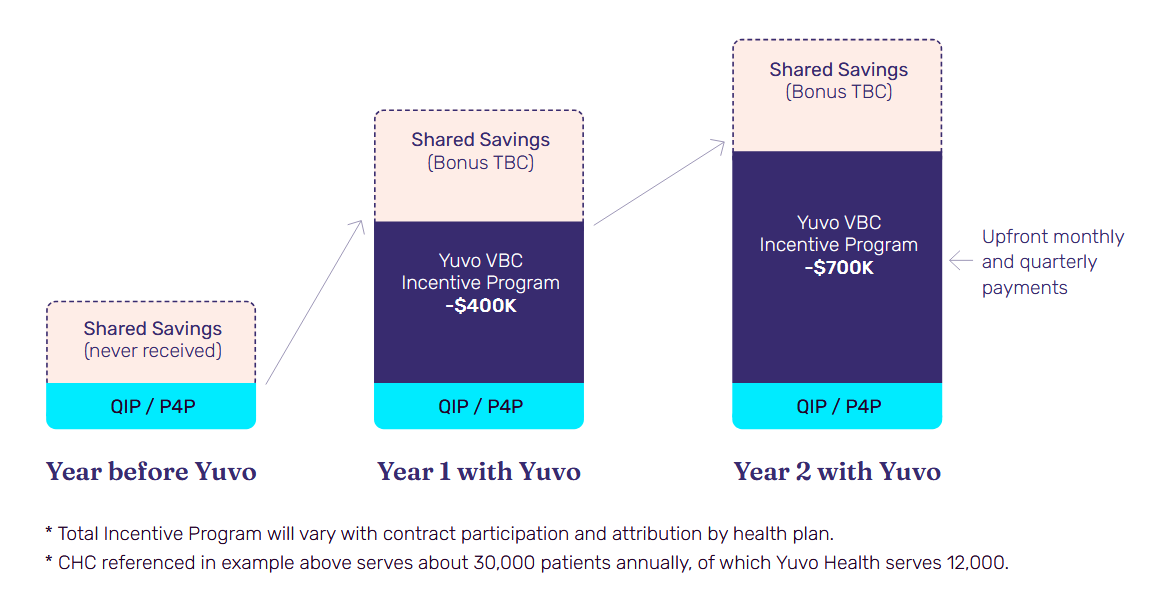
By engaging in multiple models and diversifying their reimbursement portfolio, CHCs and FQHCs can accrue additional income to expand their reach, add more services, and truly maximize their ability to serve disadvantaged and vulnerable communities.
Interested in finding success in value-based care? Download our guide.
Editor's note: This article was originally published in November 2022 and updated in December 2025.


Subscribe to our monthly newsletter just for community health centers
We’ll send occasional emails with Yuvo and FQHC news.


